Transforming Patient Intake with AI: A Real-World Triage System Case Study
Artificial intelligence in healthcare has moved from experimental pilots to mission-critical operational systems. Hospitals and speciality clinics increasingly rely on AI to streamline patient intake, enhance clinical decision support, and reduce administrative burden. However, healthcare environments impose strict requirements: safety, consistency, explainability, and alignment with real-world clinical workflows.
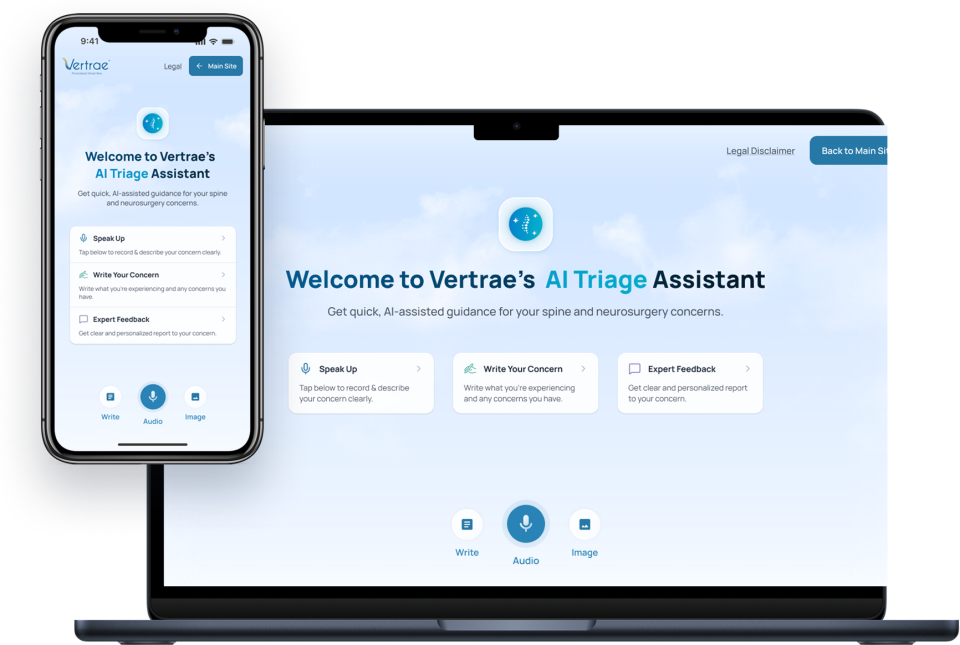
This case study documents how Impero IT Services designed, built, and stabilized a voice-driven AI triage assistant for a speciality spine and pain-management clinic. It highlights the architectural decisions, failures, pivots, and engineering insights that ultimately led to a production-ready Minimum Viable Product (MVP).
Project Overview
The objective was to create an intelligent triage assistant capable of conducting an initial patient intake conversation through natural speech. The system needed to:
Allow patients to describe symptoms conversationally Convert speech to structured text in real time
Ask clinically relevant follow-up questions
Identify potential red flags
Produce a structured summary for clinicians
Reduce front-desk workload and intake time
Ask clinically relevant follow-up questions
Unlike simple chatbots, this solution had to approximate the logic of a trained intake professional while remaining safe, consistent, and scalable.
Technology Stack
To meet both performance and compliance expectations, a modular architecture was implemented.
Frontend
- React.js for responsive UI
- TailwindCSS for rapid interface styling
- Chrome Web Speech API for real-time voice capture
The interface was intentionally minimal to reduce cognitive load for patients of varying technical proficiency.

AI Layer
- OpenAI GPT model for natural language reasoning
- Function Calling for structured AI actions
- Retrieval-Augmented Generation (RAG) for domain grounding
- Dynamic prompting for context management
This layer handled conversational intelligence, clinical logic interpretation, and response generation.

Backend
- Node.js with Express for API orchestration
- Secure session handling for conversation continuity
- Controlled AI request pipelines

Data & Deployment
- Encrypted session storage with no persistent PHI in MVP phase.
- HTTPS-secured subdomain hosting
- Strict access controls
Security and privacy considerations were embedded from day one, reflecting our disciplined approach as an MVP Development Company even at the MVP stage.
The Client Use Case
Our client, a specialized spine and pain-management clinic, faced several operational bottlenecks:
- High intake times for new patients
- Inconsistent information capture
- Staff overload during peak hours
- Difficulty prioritizing urgent cases
They required a system that could perform preliminary triage before the patient met a clinician, ensuring that appointments began with structured, actionable information.
Because healthcare intake is safety-critical, the AI system needed to be conservative, reliable, and clinically aligned rather than merely conversational.
The Development Journey
This is a phased evolution from deterministic control toward adaptive AI orchestration, shaped by real-world testing, failures, and critical architectural pivots.
Phase 1 - Starting with a Rule-Based System
The initial architecture relied on a traditional deterministic approach with a large rules engine. The design included:
Predefined conversational flows
Conditional branching logic
Instruction hierarchies
Symptom-specific pathways
This method was chosen to maintain control over clinical interactions and reduce hallucinations. network management.This method was chosen to maintain control over clinical interactions and reduce hallucinations.
On a small scale, the approach worked reasonably well.
Phase 2 - When Rules Began to Fail
As more medical scenarios were introduced, the rules of engines became increasingly fragile. The key problems emerged when:
Logical Conflicts
Multiple rules triggered simultaneously for overlapping symptoms, producing contradictory guidance.
Combinatorial Explosion
Every new condition required dozens of new rules and exceptions, rapidly increasing system complexity.
Unstable Outputs
Despite deterministic logic, interactions became inconsistent because natural language inputs rarely matched predefined patterns perfectly.
Maintenance Overhead
Updating clinical logic required manual revisions across numerous interdependent rules, creating a high risk of regression.
The system was becoming harder to control, not easier.
Phase 3 - Identifying the Root Cause
Through iterative testing, the team discovered a core issue:
Large language models do not behave optimally when constrained by excessively granular rule stacks.
Over-specification caused:
Instruction conflicts
Priority ambiguities
Reduced model reasoning effectiveness
Unpredictable conversational flow
Instead of guiding the AI, the rules were interfering with it.
Phase 4 - The Turning Point
The breakthrough came from reframing the architecture.
Rather than forcing the model to follow rigid conversational scripts, the team allowed the model to reason freely within controlled boundaries and then structured its outputs programmatically.
This required a shift from “rule enforcement” to “action orchestration.”
Phase 5 - Transition to Function Calling
The system was rebuilt using a function-calling paradigm.
Instead of embedding logic directly in prompts, the AI could invoke predefined functions representing discrete clinical tasks, such as:
Recording symptoms
Classifying pain characteristics
Detecting risk indicators
Requesting clarification
Generating structured summaries
The backend validated and executed these actions, ensuring safety and consistency.
Architectural Comparison Before vs. After
Giving you a side-by-side evaluation that highlights how foundational design choices directly influenced system reliability, scalability, and clinical usability.
Rule-Based System
An initially structured approach that prioritized explicit control through predefined logic but struggled with complexity and variability in natural patient input.
Strengths
High initial control
Predictable flows in simple cases
Limitations
Unstable at scale
Difficult to maintain
Poor adaptability to real language
Conflicting instructions
Function-Calling Architecture
A modern AI interaction model that separates reasoning from execution, enabling consistent, safe, and scalable handling of complex clinical conversations.
Advantages
Consistent behavior across scenarios
Clear separation of reasoning and execution
Easier updates to clinical logic
Reduced prompt complexity
Improved accuracy and reliability
Scalable design
The new architecture transformed the system from brittle to robust.
Real-Time Engineering Challenges
Developing healthcare AI involves constraints rarely present in consumer applications.
Complex Medical Logic
Symptoms often overlap across conditions, requiring nuanced questioning rather than linear flows.
Consistency Across Sessions
Healthcare providers require reproducible outputs. The AI needed to produce structured summaries in a standardized format regardless of conversational variations.
Safety And Risk Mitigation
The system had to avoid:
Providing diagnoses
Offering unsafe advice
Missing urgent symptoms
Guardrails were implemented to escalate concerning responses to human review.
Clinician-Ready Output
The final summary had to be immediately useful, not merely descriptive. Key elements included:
Primary complaint
Symptom duration
Pain characteristics
Functional limitations
Red flag indicators
Suggested triage category
Voice Recognition Stability
Natural speech introduces challenges such as:
Accents and speech variability
Background noise
Incomplete sentences
Self-corrections
Real-time transcription needed continuous tuning for accuracy.
How Impero Delivered Measurable Impact
The final MVP delivered value across technical, operational, and clinical dimensions.
Robust Technical Architecture
A modular design allowed independent improvement of voice capture, AI reasoning, and backend logic without system-wide disruption.
Clinical Logic Mapping
Subject-matter alignment ensured that questions reflected real intake practices rather than generic symptom checklists.
Stable AI Behavior
Function calling eliminated most unpredictable responses while preserving natural conversation quality.
Patient-Friendly User Experience
The voice interface reduced friction for patients who struggle with long forms or typing.
Scalable Foundation
The architecture supports future enhancements such as:
- EHR integration
- Multilingual capability
- Predictive triage prioritization
- Analytics dashboards
Final Results
After iterative refinement, the system achieved its core objectives:
- Consistent AI-driven symptom collection
- Smooth conversational interaction
- Structured, clinician-ready summaries
- Reduced intake burden on staff
- Improved preparation for consultations
Most importantly, the solution demonstrated that healthcare AI systems can be both intelligent and operationally dependable when engineered with the right architecture.
Key Lessons Learned
This project produced several insights applicable to any healthcare AI initiative delivered by our AI-Powered Mobile App Development Company. This architecture supports deployment in mobile apps, web platforms, and desktop applications.


Over-constraining language models reduces reliability


Structured actions outperform rigid scripts


Clinical alignment is as important as technical accuracy


Safety mechanisms must be built in from the start


Voice interfaces introduce unique engineering challenges


MVP success depends on operational usefulness, not feature count
Conclusion
Building AI for healthcare requires more than advanced models; it demands architectural discipline, domain understanding, and iterative experimentation.
The transition from a rule-heavy system to a function-oriented architecture proved decisive. By allowing the AI to reason naturally while constraining execution through structured actions, Impero delivered a triage assistant that is precise, stable, and scalable.
This project underscores a broader principle that a successful healthcare AI does not replace human judgements but augments clinical workflows with reliable, intelligent tools. As AI adoption accelerates across the medical sector, systems built on these principles will form the backbone of next-generation patient intake and decision support.

Author
Dhara Shah
Dhara Shah is a detail-oriented Quality Assurance Engineer with a strong background in information technology. Carrying her deep experience in testing and analysis, she now focuses on coordinating teams, optimizing workflows, and ensuring projects are delivered efficiently and on schedule. Dhara is known for her collaborative approach, responsiveness, and ability to align cross-functional efforts toward shared goals. She brings along a structured, results-driven mindset to every initiative she leads.
Begin Your Next Phase of Digital Growth
Collaborate with a technology partner that understands your business goals and delivers solutions built for scale, security, and long-term success.
Schedule a Consultation